Intra-abdominal Infections
Appendicitis & Infections of the Liver and Biliary System
2026-03-01
Intraabdominal Infections, Part 2
Prof. Russell E. Lewis
Department of Molecular Medicine
University of Padua
russelledward.lewis@unipd.it
https://github.com/Russlewisbo
slides available at: www.padovaid.com
 |
What is appendicitis?
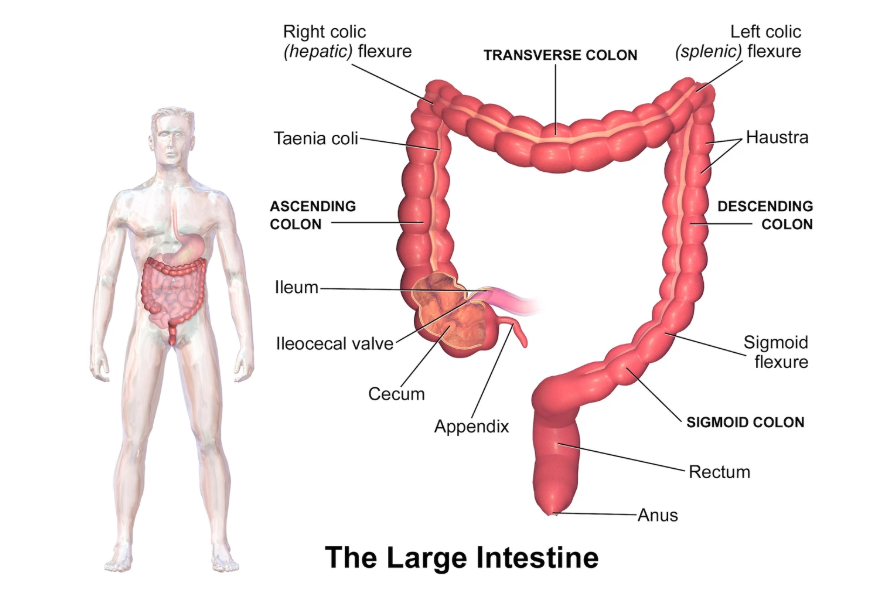
Anatomy of the appendix
- Tube-shaped structure, 5–10 cm long
- Arises 2–3 cm below terminal ileum
- Medial posterior wall of cecum
- Common atypical positions: descending pelvic, transverse retrocecal, ascending postileal
The Appendix: Not just vestigial
Epidemiology: By the Numbers
Age and Sex Distribution
- Peak incidence: 15–25 years
- Rare in infants
- Declines after age 45 (<25% of cases)
- Male-to-female ratio: 1.4:1
- Most common surgery for individuals ≤17 years
Geographic Variation
- Lower incidence in rural, non-industrialized areas
- Incidence of appendicitis increases with industrialization
- Similar pattern seen with diverticulitis
- Estimated lifetime risk <1% in rural sub-Saharan Africa
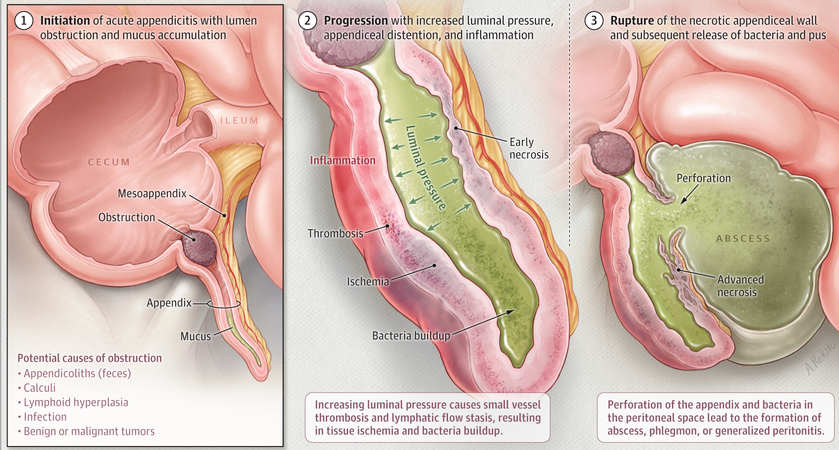
Classic pathogenesis model
Challenging the classic pathology model
The dietary fiber hypothesis
Microbiology: Culture-based
10–14 organisms typically can be cultured from inflamed appendix
Reflects colonic microbiota
Key organisms:
Escherichia coli
Bacteroides fragilis group
Prevotella spp.
Peptostreptococcus spp.
Streptococcus anginosus group
Microbiology: 16S rRNA Insights
Appendiceal microbiome is remarkably diverse
Dozens of phyla, hundreds of species
Distinct from other GI tract locations
Enriched in inflamed appendix:
Fusobacterium
Peptostreptococcus
Parvimonas
Dysbiosis may drive appendicitis (not obstruction)
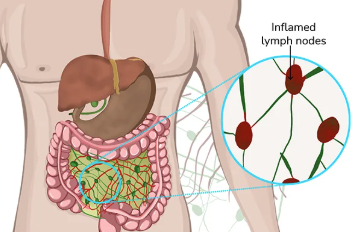
Mimics of appendicitis: Mesenteric adenitis
Mimics of appendicitis: Specific pathogens to know
| Organism | Presentation |
|---|---|
| Yersinia spp. | Ileocecitis, mesenteric adenitis → mimics appendicitis |
| Campylobacter | Pseudoappendicitis with ileocecitis |
| Salmonella | Pseudoappendicitis with mesenteric adenitis |
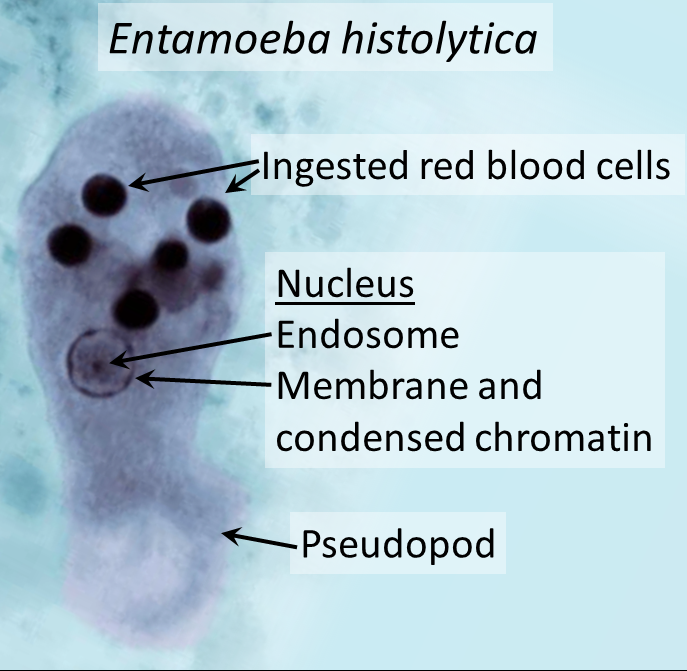
| Entamoeba histolytica (protozoan parasite) | True appendicitis (rare) |
| Viruses (EBV, CMV, measles) | Mesenteric adenitis |
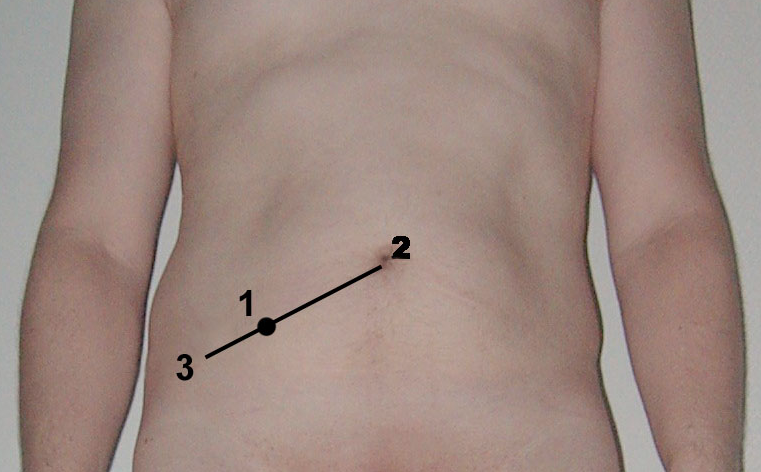
Classic clinical presentation
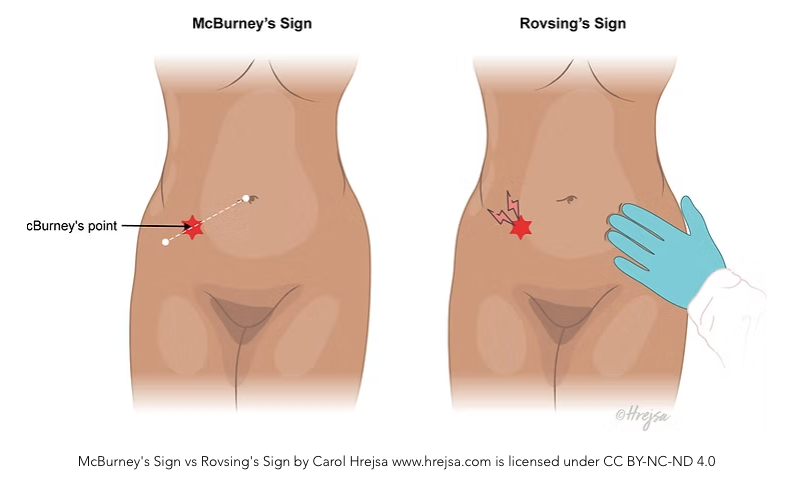
Rovsing sign
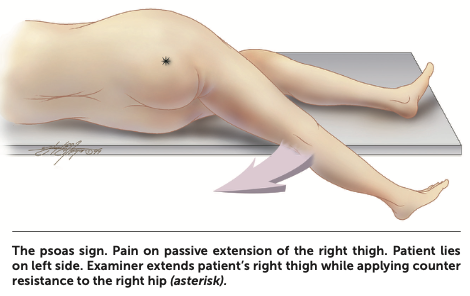
Psoas sign
 |
 |
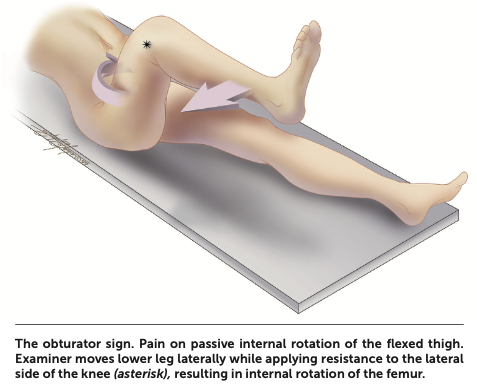
Obturator sign
Physical examination signs
| Sign | Description |
|---|---|
| Rovsing sign | RLQ pain with LLQ palpation |
| Psoas sign | Pain with active hip extension |
| Obturator sign | Pain with internal hip rotation |
| Guarding (tense abdominal wall) | Involuntary muscle contraction |
| Rebound tenderness | Pain on release of pressure |
Diagnostic Challenges
Warning
Diagnosis is more difficult in:
Women of childbearing age (gynecologic mimics)
Pelvic appendixes (pelvic/LLQ pain)
Third-trimester pregnancy (RUQ pain shift)
Elderly patients (atypical presentations)
Young children (inability to localize pain)
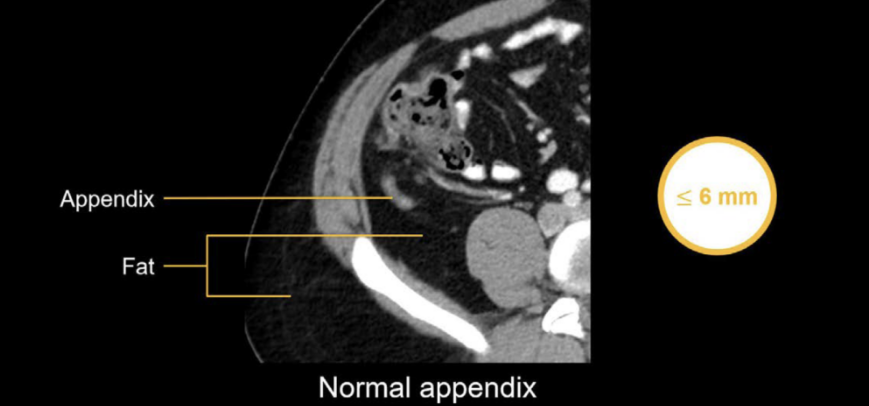
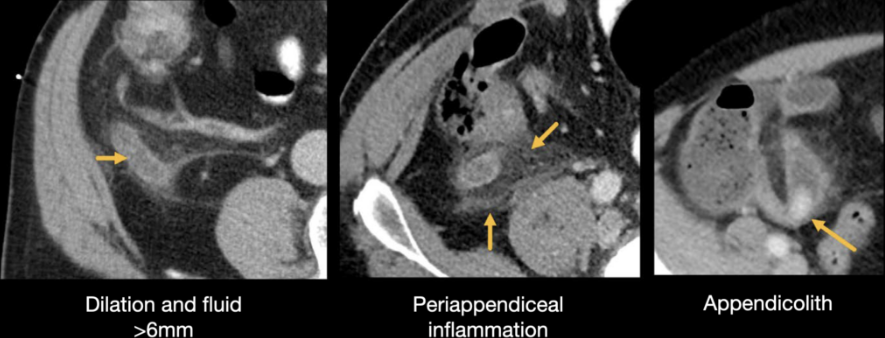
CT Imaging: Normal vs. abnormal
Imaging
- CT with IV contrast: Sensitivity and specificity both >95%
- Preferred in adults
- Dilated appendix >6 mm, peri-appendiceal fat stranding
- Ultrasonography: First-line in children and pregnant women
- Sensitivity 70–90%
- MRI: Alternative in pregnancy
Scoring systems
Alvarado Score (MANTRELS): migration, anorexia, nausea, tenderness, rebound, elevated temp, leukocytosis, shift to left
| Letter | Clinical Feature | Points |
|---|---|---|
| M | Migration of pain to right lower quadrant | 1 |
| A | Anorexia | 1 |
| N | Nausea/vomiting | 1 |
| T | Tenderness in right lower quadrant | 2 |
| R | Rebound pain | 1 |
| E | Elevated temperature (>37.3°C) | 1 |
| L | Leukocytosis (>10,000/mm³) | 2 |
| S | Shift to left (neutrophilia >75%) | 1 |
Alvarado Score (MANTRELS): Interpretation
| Score | Risk | Recommendation |
|---|---|---|
| 1–4 | Low | Appendicitis unlikely; consider discharge with observation |
| 5–6 | Equivocal/intermediate | Further workup warranted (imaging, observation, surgical consult) |
| 7–8 | High | Likely appendicitis; surgical consultation indicated |
| 9–10 | Very high | Appendicitis highly probable; proceed to surgery |
IR Score (Appendicitis Inflammatory Response):
| Variable | Criteria | Points |
|---|---|---|
| Vomiting | Present | 1 |
| Right lower quadrant pain | Present | 1 |
| Rebound tenderness or muscular defense | Mild | 1 |
| Moderate | 2 | |
| Strong | 3 | |
| Temperature | ≥ 38.5°C | 1 |
| Leukocytosis (×10⁹/L) | 10.0–14.9 | 1 |
| ≥ 15.0 | 2 | |
| Proportion of neutrophils (%) | 70–84% | 1 |
| ≥ 85% | 2 | |
| CRP (mg/L) | 10–49 | 1 |
| ≥ 50 | 2 |
IR score interpretation
Interpretation
| Score | Risk | Recommendation |
|---|---|---|
| 0–4 | Low | Appendicitis unlikely; discharge with observation |
| 5–8 | Indeterminate | Imaging, active observation, or surgical consult |
| 9–12 | High | Appendicitis highly probable; surgical intervention |
Key advantages over Alvarado
CRP is included — a more sensitive and specific acute-phase reactant than WBC alone
Graded variables — rebound tenderness, PMN%, WBC, and CRP are each weighted by severity rather than binary yes/no
Higher specificity for ruling in appendicitis, and better negative predictive value for low scores
Performs well in both sexes, with some studies showing superior performance to Alvarado in women
Validated in multiple prospective European and international cohorts
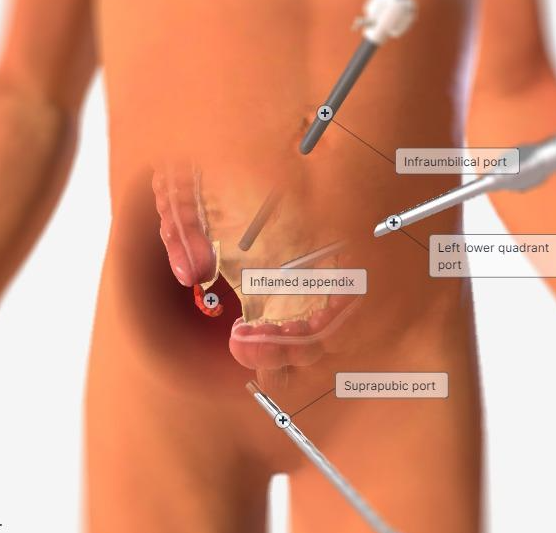
Treatment: Surgical
An uncomplicated surgery?
Treatment: Antibiotic-first strategy
Tip
An “antibiotic first” strategy has emerged as a safe and effective option for uncomplicated appendicitis
- Avoids surgery in ~60–70% of patients
- Outcomes comparable to appendectomy
- Recurrence rate ~25–30% at 5 years
- Patient selection is key: uncomplicated, no fecalith
Antibiotic regimens for appendicitis
- Uncomplicated: Piperacillin-tazobactam or ceftriaxone + metronidazole
- Perforated: IV antibiotics 3–5 days → oral step-down
- Duration guided by clinical response
- Ensure anaerobic coverage (metronidazole)
Appendicitis: Key takeaways
- Most common surgical emergency of the abdomen
- Classic: periumbilical pain → RLQ migration
- CT is the imaging gold standard in adults
- Laparoscopic appendectomy remains definitive treatment
- Antibiotic-first strategy: valid for uncomplicated cases
- Microbiome dysbiosis: emerging pathogenic concept
Infections of the liver
and biliary system
Liver abscess: Two categories
| Feature | Amebic | Pyogenic |
|---|---|---|
| Cause | Entamoeba histolytica | Bacterial (polymicrobial or monomicrobial) |
| Pathology | Hepatocyte apoptosis | Suppurative infection |
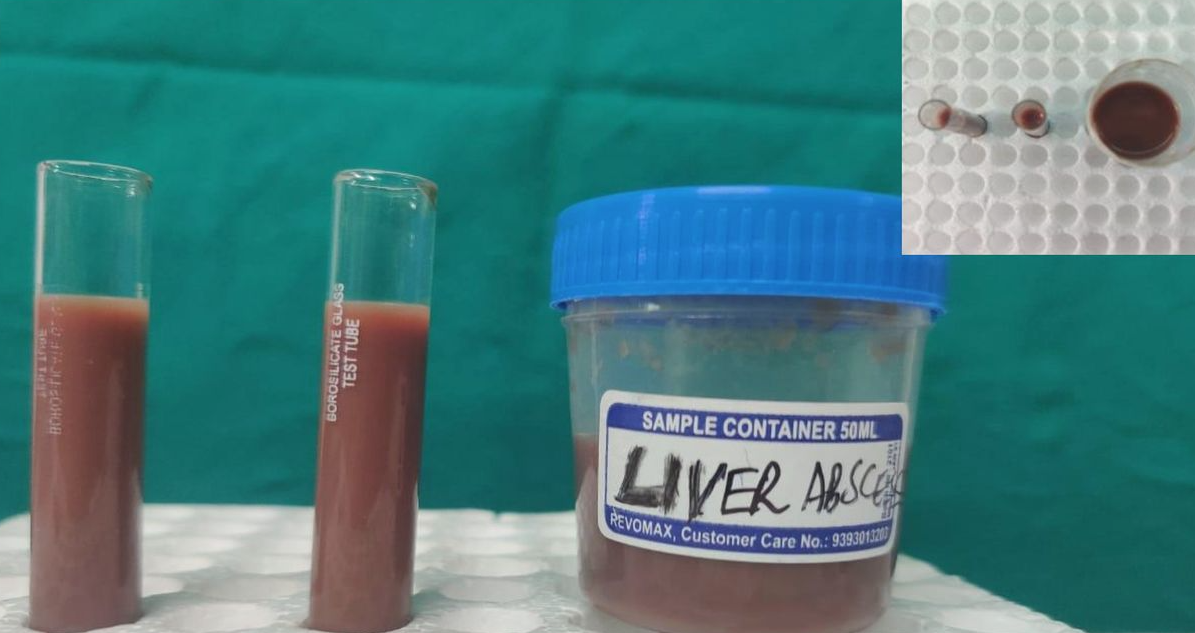
| “Pus” appearance | Anchovy paste (nonpurulent) | Purulent |
| Primary treatment | Medical (metronidazole) | Drainage + antibiotics |
Amebic Liver Abscess: Epidemiology
- Rare in the US (travelers, immigrants, MSM)
- 2,983 total cases of amebiasis in 1994
- Annual incidence decreasing 2.4% per year
- Worldwide: E. histolytica second only to malaria as cause of death from parasitic disease
- Male: female ratio = ranging from 5–18 : 1 in epidemiological studies
E. histolytica vs. E. dispar
Pyogenic liver abscess: epidemiology
- Incidence: 1–4 per 100,000 annually (US/Europe)
- In Asia: 5–10× higher (community-acquired K. pneumoniae)
- Peak: 5th–6th decades of life
- 50% solitary; right lobe most common
- Biliary disease: now the leading cause
Routes of hepatic invasion
| Route | Frequency |
|---|---|
| Biliary tree (cholangitis) | 40–50% |
| Cryptogenic | 20–40% |
| Portal vein (pylephlebitis) | 5–15% |
| Hepatic artery (bacteremia) | 5–10% |
| Direct extension | 5–10% |
| Trauma | 0–5% |
Risk factors for pyogenic liver abscess
- Diabetes mellitus: >3× risk
- Biliary disease (gallstones, obstruction)
- Hepatobiliary procedures
- Chronic granulomatous disease
- Hemochromatosis (especially Yersinia) -iron sequestration in liver
- Malignancy
- Cirrhosis
- Immunosuppression
Pathogenesis: Amebic liver abscess
“Anchovy paste” from liver abscess
Virulence Factors of E. histolytica
| Factor | Function |
|---|---|
| Gal/GalNAc lectin | Epithelial adherence |
| Amoebapores | Pore formation in target cell membranes |
| Cysteine proteases | Tissue invasion, immune evasion |
| Apoptosis induction | Hepatocyte and neutrophil killing |
Host Factors in Amebic Liver Abscess
- HLA-DR3: increased susceptibility
- Testosterone: risk factor (10× higher in men)
- Host defense mechanisms:
- Complement
- Neutrophils
- Interferon-γ
- Nitric oxide
- Adaptive immunity
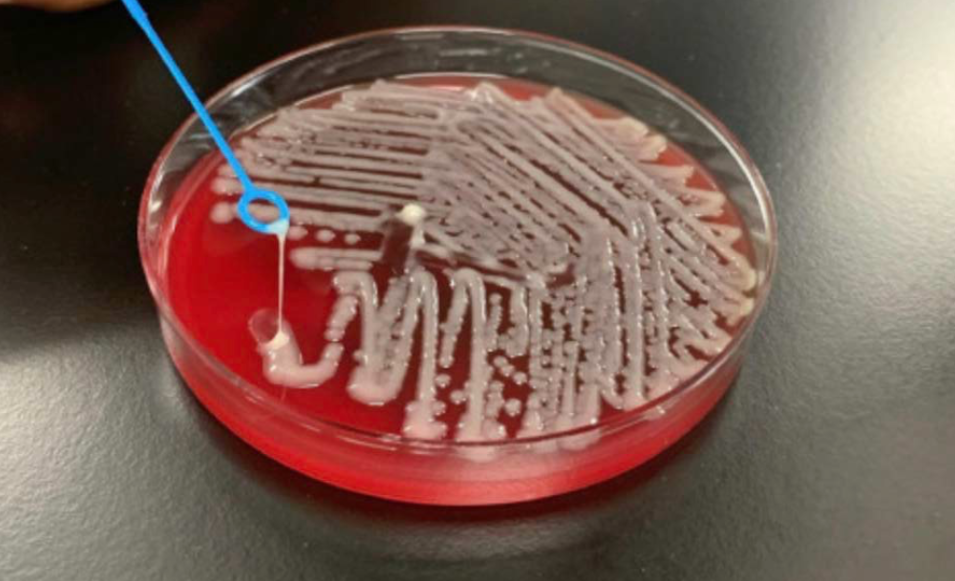
Microbiology of Pyogenic Liver Abscess
Cultures positive in 80–90% of cases
Polymicrobial in 20–50% , key organisms:
E. coli and K. pneumoniae (most common gram-negatives)
Streptococcus anginosus group (most common gram-positive)
Bacteroides spp. (most common anaerobe)
Anaerobes recovered in 15–30%
Epidemic Klebsiella pneumoniae liver abscess
K. pneumoniae virulence determinants
- Capsular polysaccharide (K1/K2 serotypes)
- magA gene → hypermucoviscosity
- cps gene cluster (25-kb chromosomal element)
- RmpA (mucoid phenotype regulator)
- Aerobactin (iron acquisition)
- Virulence plasmids (pLVPK, pK2044)
Convergent drug-resistant K. pneumoniae
Warning
Public Health Threat
- Classic hypervirulent strains: typically drug sensitive
- MDR/XDR strains can acquire virulence plasmids
- Or hypervirulent strains can acquire resistance plasmids
- Fatal ventilator-associated pneumonia outbreaks in China
- Only a minority currently show hypervirulent phenotypes in lab
Clinical features: Amoebic liver abscess
Fever + dull, aching RUQ pain
Only 15–35% have GI symptoms
Acute (<2 weeks) in ~2/3 of cases
Can develop months to years after travel
Risk factors: male sex, corticosteroid use
Indistinguishable from pyogenic on clinical grounds alone
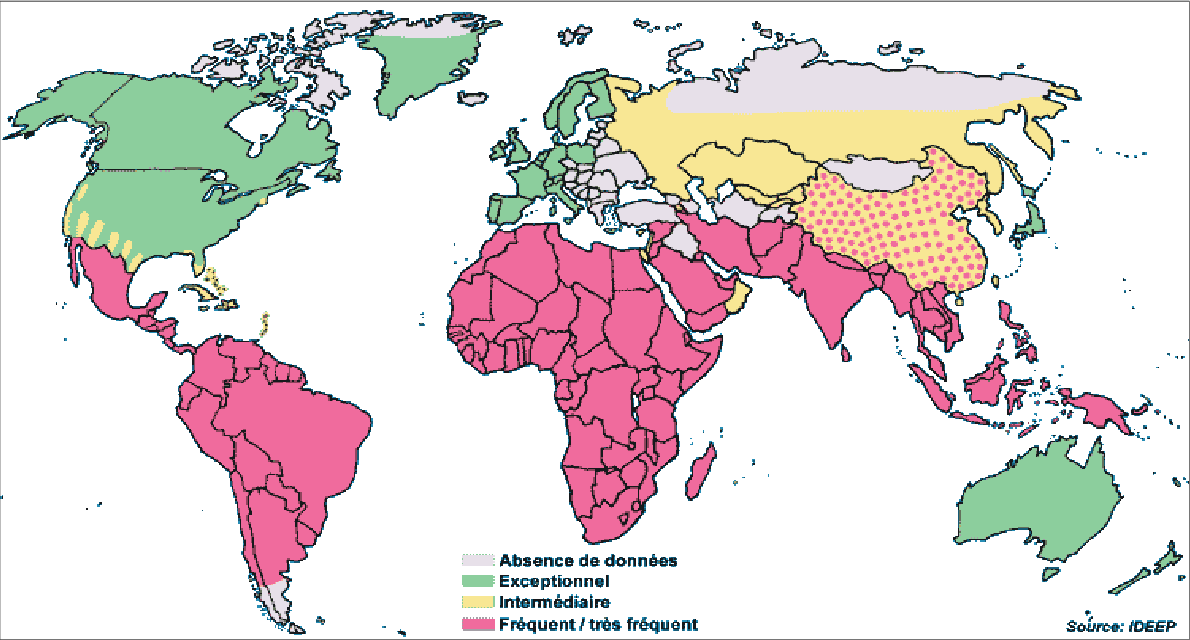
Endemic areas for amebic liver abscess
Clinical Features: Pyogenic Liver Abscess
- Classic triad (fever, jaundice, RUQ tenderness) in only 10%
- Most common: fever without localizing signs
- General failure to thrive
- Malaise, fatigue, anorexia, weight loss
- Hematogenous abscesses present most acutely (3 days)
- Pylephlebitis (portal vein) -related abscesses: longest duration (42 days)
Comparing amoebic vs. pyogenic liver abscess
| Feature | Amebic | Pyogenic |
|---|---|---|
| Male:female | 5–18:1 | 1–2.4:1 |
| Age | 30–40 | 50–60 |
| Duration (days) | <14 | 5–26 |
| Mortality | 10–25% | 0–5% |
| Abdominal pain | 80% | 55% |
| RUQ tenderness | 75% | 25–55% |
Diagnosis: Laboratory findings
- Leukocytosis: present in most patients (75–80%)
- Elevated alkaline phosphatase: most common abnormal LFT (~2/3)
- Normal value does not exclude diagnosis
- Transaminases: generally mildly elevated
- Procalcitonin: typically elevated
- Albumin and prothrombin time: usually normal
Diagnosis: imaging
| Modality | Sensitivity | Best For |
|---|---|---|
| Ultrasonography | 70–90% | Initial assessment, biliary disease |
| CT (contrast-enhanced) | ~95% | Definitive diagnosis, drainage guidance |
| MRI | High | Distinguishing from neoplasia |
| Fine-needle aspiration | Definitive | Diagnostic confirmation |
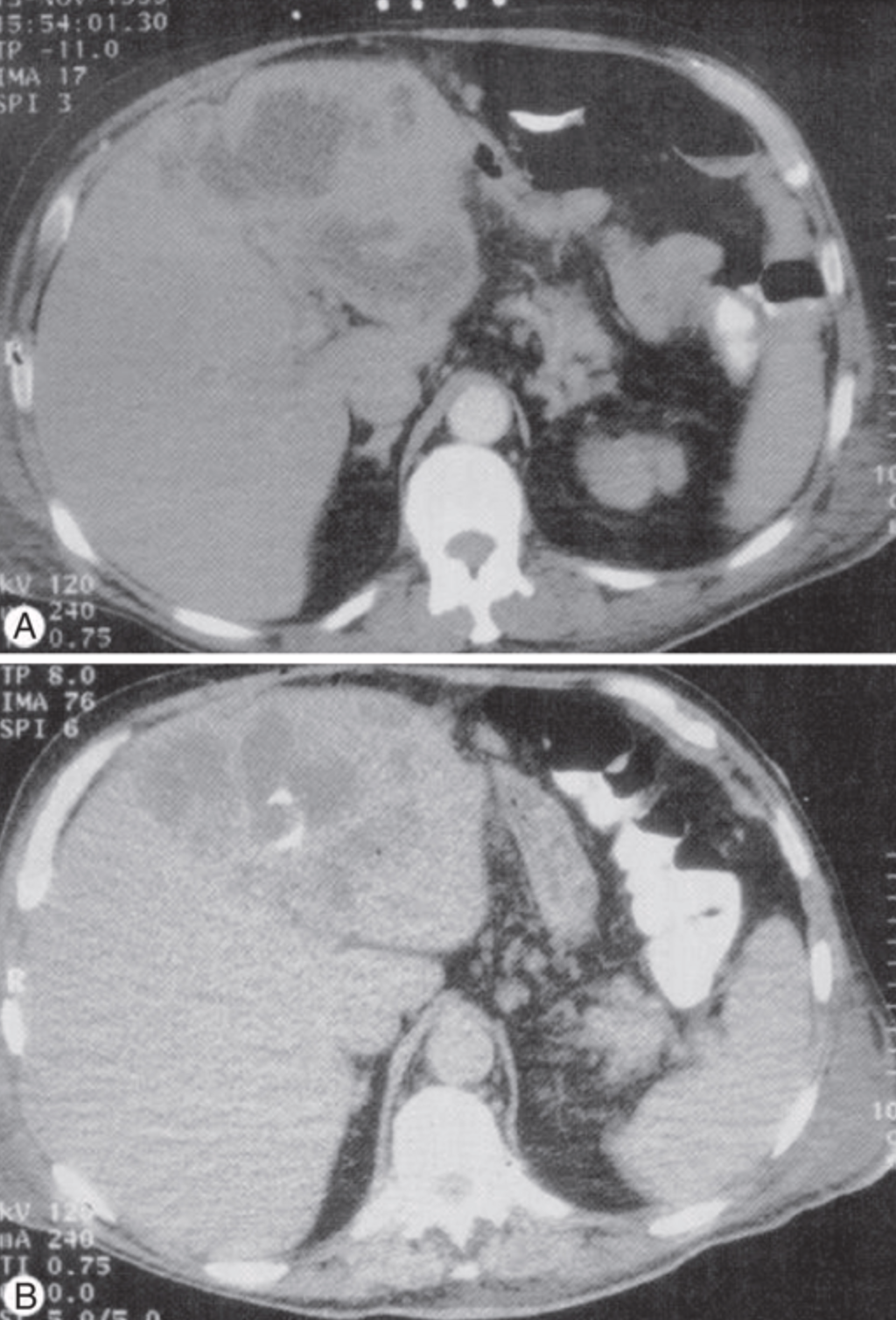
Diagnosis CT imaging
Diagnosis: amoebic serology
Enzyme immunoassay: sensitivity 65–92%, highly specific
Can be negative if symptom duration <2 weeks
Repeat serology in 1–2 weeks usually positive
Positive serology confirms present or prior infection
Cannot distinguish from extraintestinal disease
ELISA for Gal/GalNAc lectin: >95% sensitivity in serum
Emerging diagnostics
- Molecular multiplex panels:
Highly sensitive for amebic colitis
Patients with liver abscess usually don’t have concurrent intestinal infection
PCR: Potential for aspirated fluid; limited to research labs
cfDNA testing: Circulating cell-free DNA
Recent study: 90% sensitivity, 100% specificity for amoebic abscess
Noninvasive blood-based assay
Treatment: Amoebic liver abscess — Medical therapy
Tip
Almost always treatable with medical therapy alone
| Drug | Regimen |
|---|---|
| Metronidazole | 750 mg TID × 7–10 days |
| Tinidazole | 2 g daily × 3 days |
| Secnidazole/Ornidazole | Extended half-life alternatives |
| Paromomycin (luminal agent) | Follow-up to eliminate colonization |
Treatment: When to drain amoebic abscess
Uncomplicated: drainage NOT required
Indications for drainage:
No response to medical therapy (>5–7 days)
Diagnostic uncertainty (rule out pyogenic)
Large lesions at risk for rupture
Left-sided abscesses — erosion through diaphragm (pericardial rupture risk)
Bacterial superinfection (1–5% of cases)
Percutaneous preferred over surgical drainage
Treatment: Pyogenic liver abscess — Drainage
Percutaneous catheter drainage: Preferred primary therapy
Success rate: 69–90%
Can be performed at time of diagnosis
Catheter left in place 5–14 days until drainage resolves
Recent success rates with antibiotics: 80–95% (even for >10 cm abscesses)
Surgical drainage if: percutaneous fails, concurrent surgical disease, multiple/loculated abscesses
Treatment: Pyogenic liver abscess — Antibiotics
| Approach | Agents |
|---|---|
| Monotherapy | Piperacillin-tazobactam OR carbapenem |
| Combination | 3rd/4th-gen cephalosporin + metronidazole OR fluoroquinolone + metronidazole |
Antibiotic Duration: An open question
No RCTs establishing optimal duration
Meta-analysis: pooled mean 32.7 days
Traditional: IV 2–3 weeks → oral 4–6 weeks total
Some evidence for shorter courses (2–4 weeks)
Singapore RCT: 4-week oral ciprofloxacin noninferior to 4-week IV ceftriaxone for K. pneumoniae
Follow-up imaging to guide duration
Aspiration vs. catheter drainage
| Feature | Aspiration | Catheter Drainage |
|---|---|---|
| Success rate | 58–88% (≤5 cm) | 69–90% |
| Recurrence | Higher | Lower |
| Meta-analysis evidence | Drainage superior | Drainage superior |
| Best for | Small, solitary abscesses | Larger, multiple abscesses |
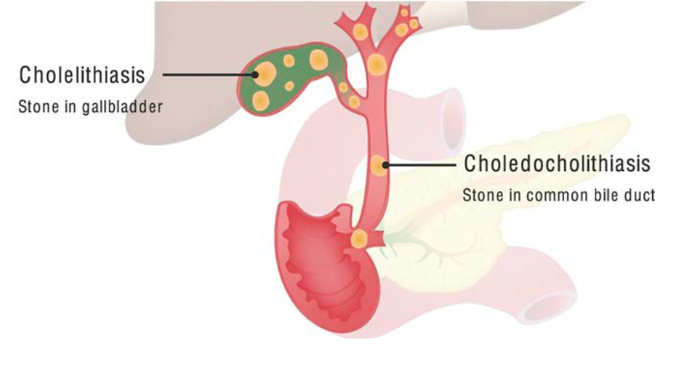
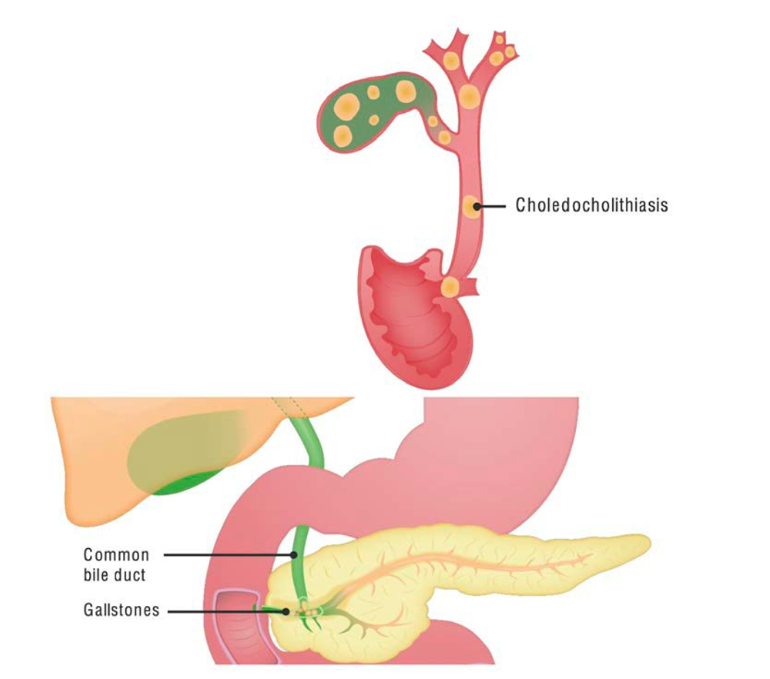
Biliary tract infections
Biliary system infections: Overview
Infections associated with
obstruction to bile flowGallstones: common and usually asymptomatic
1% to 4% complicated by acute cholecystitis
Over 100,000 cholecystectomies per year in Italy
2–15% of cases are acalculous cholecystitis
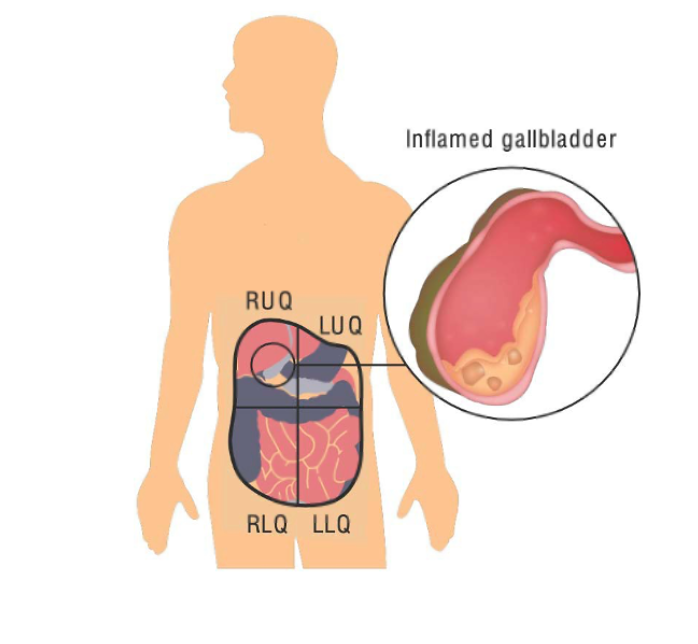
Cholecystitis: Key points
- Inflammation/bacterial infection of the gallbladder
- Usually from obstructing gallstones
- Acalculous cholecystitis: similar process without stones
- Treatment: cholecystectomy + antibiotics
- Mortality higher in acalculous cases
Diagnosis of cholecystitis
Tokyo Guidelines 2018 — Diagnostic criteria (2 of 3 categories required):
| Category | Criteria |
|---|---|
| A. Local inflammation | Murphy’s sign; RUQ pain, tenderness, or mass |
| B. Systemic inflammation | Fever; elevated CRP; elevated WBC (>10,000/mm³) |
| C. Imaging | Findings consistent with acute cholecystitis |
Imaging modalities
| Modality | Key findings | Sensitivity / Specificity |
|---|---|---|
| Ultrasound (first-line) | Wall thickening (>4 mm), pericholecystic fluid, sonographic Murphy’s sign | ~80% / ~80% |
| CT | Wall thickening, pericholecystic stranding, distension | ~94% / ~59% |
| HIDA scan | Non-visualization of gallbladder | ~97% / ~87% |
Cholangitis: Key points
- Inflammation/infection of the bile ducts
- Charcot triad: fever, jaundice, RUQ pain
- Reynolds pentad: Charcot triad + hypotension + altered mental status (sepsis)
- Life-threatening emergency requiring urgent biliary decompression
not an encapsulated infection and will spill over to abdomen and bloodstream - Mortality: 5–10% with treatment; up to 90% without surgical and antibiotic treatment
Diagnosis of cholangitis
Tokyo Guidelines 2018 — Diagnostic criteria
| Step | Criteria |
|---|---|
| Suspected (≥1 of A + B or C) | |
| A. Systemic inflammation | Fever/chills; WBC <4 or >10 ×10⁹/L; elevated CRP |
| B. Cholestasis | Jaundice (bilirubin ≥2 mg/dL); elevated ALP, GGT, AST, ALT |
| C. Imaging | Biliary dilatation; evidence of etiology (stricture, stone, stent) |
| Definitive | One criterion from each of A, B, and C |
Severity grading (Tokyo 2018)
| Grade | Definition |
|---|---|
| Grade I (Mild) | Responds to initial antibiotic therapy; no organ dysfunction |
| Grade II (Moderate) | Abnormal WBC, fever, age ≥75, bilirubin ≥5 mg/dL, hypoalbuminemia — biliary drainage within 24–48 h |
| Grade III (Severe) | Organ dysfunction (cardiovascular, neurologic, respiratory, renal, hepatic, hematologic) — urgent drainage |
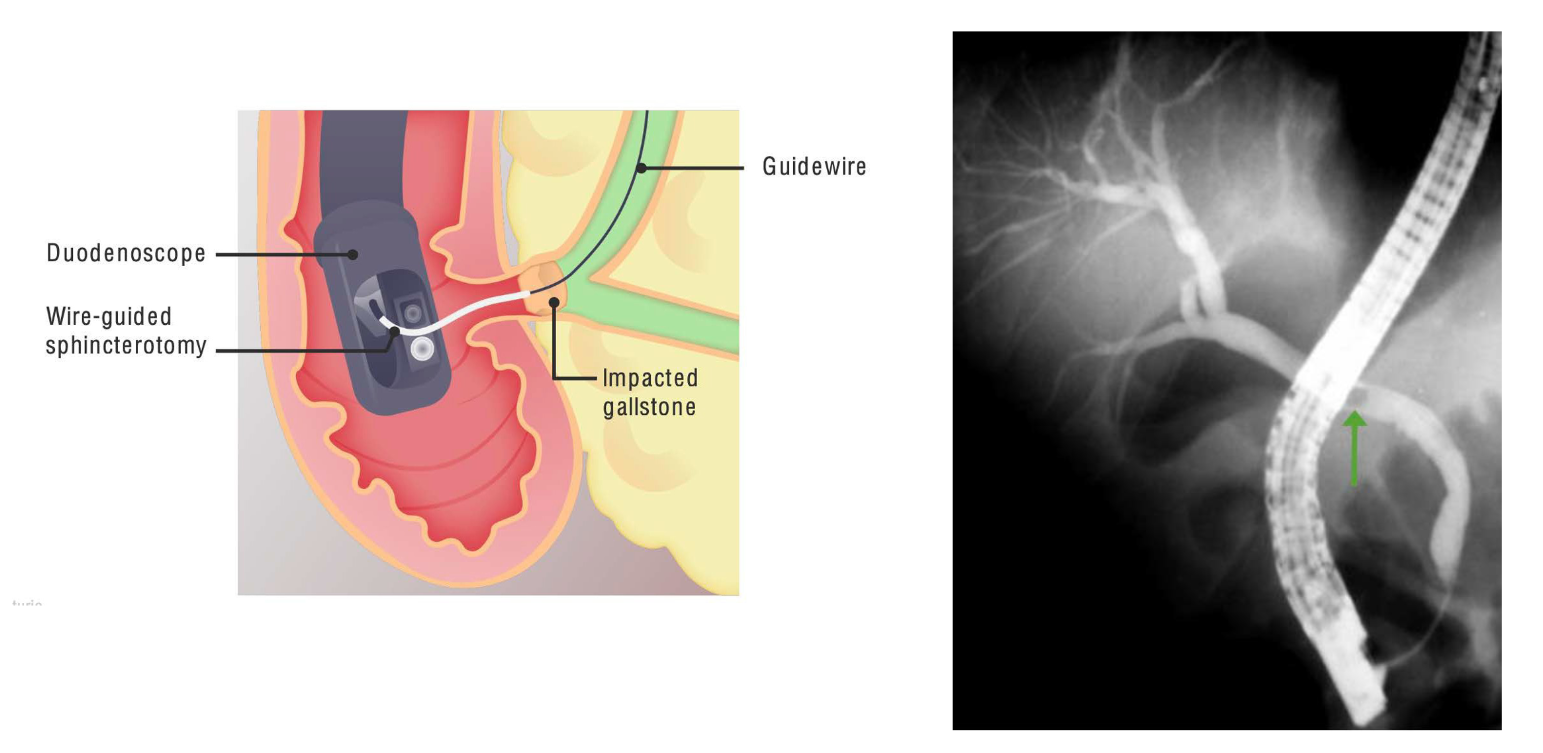
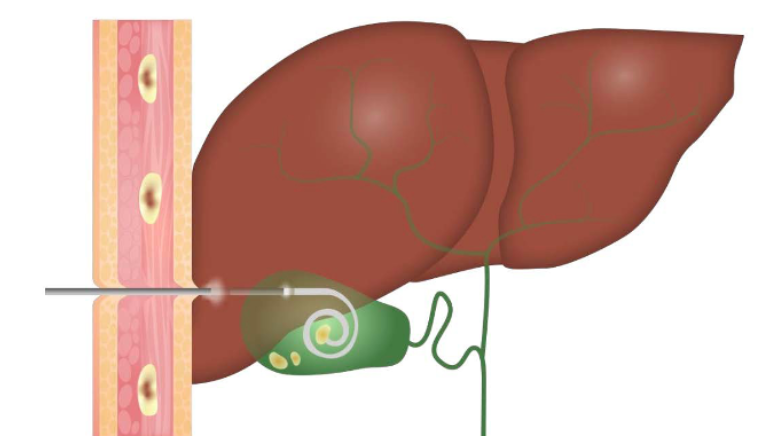
ERCP or percutaneous transhepatic drainage
Antibiotic therapy biliary tract infections
| Good Penetration (ABSCR ≥1) | ABSCR | Low Penetration (ABSCR <1) | ABSCR |
|---|---|---|---|
| Piperacillin/tazobactam | 4.8 | Ceftriaxone | 0.75 |
| Tigecycline | >10 | Cefotaxime | 0.23 |
| Amoxicillin/clavulanate | 1.1 | Meropenem | 0.38 |
| Ciprofloxacin | >5 | Ceftazidime | 0.18 |
| Ampicillin/sulbactam | 2.4 | Vancomycin | 0.41 |
| Cefepime | 2.04 | Amikacin | 0.54 |
| Levofloxacin | 1.6 | Gentamicin | 0.30 |
| Penicillin G | >5 | ||
| Imipenem | 1.01 |
ABSCR = Antibiotic Bile/Serum Concentration Ratio. Source: Ansaloni et al. PMID 27307785
Biliary tract infections: Mild–moderate severity
Community-acquired
No prior biliary instrumentation
Low resistance risk
| Regimen | Agents |
|---|---|
| 3rd-gen cephalosporin | Ceftriaxone, cefotaxime |
| 2nd-gen cephalosporin | Cefuroxime |
| 1st-gen cephalosporin | Cefazolin (cholecystitis only) |
| Fluoroquinolone | Ciprofloxacin, levofloxacin (if local resistance permits) |
| β-lactam/β-lactamase inhibitor | Amoxicillin/clavulanate |
Note
Anaerobic coverage not required unless bilioenteric anastomosis or prior biliary intervention
Biliary Tract Infections: Severe / Healthcare-Associated
Grade III cholangitis
Prior instrumentation
Healthcare-acquired
High resistance risk
| Regimen | Agents |
|---|---|
| Carbapenem | Imipenem/cilastatin, meropenem, ertapenem |
| β-lactam/β-lactamase inhibitor | Piperacillin/tazobactam |
| Fluoroquinolone + anaerobic cover | Ciprofloxacin or levofloxacin + metronidazole |
Additional considerations:
- Add vancomycin if MRSA risk (prior MRSA, healthcare-associated)
- Add fluconazole if Candida risk (immunosuppressed, prolonged prior antibiotics)
- Adjust for local antibiogram — fluoroquinolone resistance in E. coli >10% in many centers
Summary: Comparing hepato-biliary infections
| Appendicitis | Amebic Abscess | Pyogenic Abscess | |
|---|---|---|---|
| Peak age | 15–25 | 30–40 | 50–60 |
| Cause | Obstruction/dysbiosis | E. histolytica | Biliary/polymicrobial |
| Diagnosis | CT | Serology + imaging | Culture + imaging |
| Treatment | Surgery or antibiotics | Metronidazole | Drainage + antibiotics |
Summary: Comparing biliary tract infections
| Cholecystitis | Cholangitis | |
|---|---|---|
| Structure | Gallbladder | Bile ducts |
| Cause | Gallstone obstruction; acalculous in critically ill | Biliary obstruction (stones, stricture, malignancy) |
| Clinical features | Fever, RUQ pain, Murphy’s sign | Charcot triad (fever, jaundice, RUQ pain); Reynolds pentad if septic |
| Urgency | Urgent (elective if mild) | Medical emergency — biliary decompression within 24–48 h |
| Diagnosis | Ultrasound ± CT | Clinical + ultrasound/MRCP/CT |
| Microbiology | E. coli, Klebsiella, Enterococcus | Same + anaerobes if bilioenteric anastomosis |
| Source control | Cholecystectomy (laparoscopic preferred) | ERCP or percutaneous transhepatic drainage |
| Antibiotics — mild | Cefazolin, ceftriaxone, amoxicillin/clavulanate | 3rd-gen cephalosporin, fluoroquinolone |
| Antibiotics — severe | Piperacillin/tazobactam, carbapenem | Piperacillin/tazobactam, carbapenem ± vancomycin |
| Mortality | <1% (calculous); higher in acalculous | 5–10% treated; up to 90% without decompression |